As I discussed in my last post, so many SIBO sufferers and practitioners mistakenly view SIBO as solely a bacterial problem. By blindly focusing on the overgrowth, many SIBO sufferers relapse continuously, because they haven’t addressed the motility problem that is causing their SIBO.
These motility problems can stem from a plethora of potential root causes such as hormonal dysfunction (especially thyroid diseases like Hashimotos and cortisol dysregulation), large intestinal bacterial imbalances, autoimmune diseases, liver inflammation, heavy metal toxicity and brain inflammation (I know there are more causes, but these are the biggies). In this article, I want to shed some light on how brain inflammation can cause disturbances in motility and MMC function.
All the experts seem to agree that a deficiency in the Migrating Motor Complex (MMC) activity is the underlying cause of SIBO. While it is common for practitioners to prescribe prokinetics to support MMC function, it doesn’t seem like a lot of practitioners focus specifically on repairing the system that generates MMC activity: the brain-gut axis.
I want to preface this article by pointing out that not everyone’s SIBO case is rooted in a brain-gut axis dysfunction. But because the brain is so intimately connected with the gut, once your gut is on fire due to SIBO, it is only a matter of time before your brain catches on fire too (figuratively speaking). The key takeaway here is that we could all benefit by taking steps to keep our brains healthy when dealing with any gut issues, not just SIBO.
This relationship isn’t linear either, meaning that inflammation that originates in the brain will eventually effect the gut. Individuals with brain injuries and neurodegeneration (even natural degeneration that comes with aging) will develop delayed gut motility and intestinal permeability (leaky gut). In fact, when scientists induce a traumatic brain injury in lab animals, they can develop leaky guts in as little as 6 hours!
Most of the info in this article on the brain gut axis is from Datis Kharrazian’s work. Datis is an expert in functional neurology and just an all around bad ass! Please check out his book, “Why isn’t my Brain Working?”, if you want a deeper education about the brain-gut connection. You can also check out this presentation where he addresses SIBO and brain health directly. More recently, I heard his talk at the recent SIBO SOS summit and was again blown away by his brilliance yet again! Also, there is a rumor floating around that he is writing a SIBO book, which would be amazing! Now that I have successfully fan girled Datis….we can jump into more on what the brain-gut axis is and how to fix it.

What is the Brain-Gut Axis? Why is it important?
The Brain-Gut axis is the term used to describe the dynamic and intimate communication network between the brain and the gut. In my mind when I think of this connection, I always picture two best friends that tell each other everything. They share all their dirty secrets and their emotional happiness rests on the happiness of the other. If your best friend is sad, you are going to feel sad. The same type of relationship occurs between the gut and the brain. Information is constantly being delivered to the brain from the gut and the brain interprets this information and sends messages back to the gut. If the brain isn’t happy, the gut isn’t happy (and vice versa).
It can be easy to forget the brains vital role in digestion and SIBO recovery when we are narrowly focused on killing the overgrowth! But, the brain is responsible for triggering autonomic processes that are essential for healthy digestive function. The brain controls motility, digestive enzyme release and regulates blood flow and nutritional support to the GI tract ensuring that it stays healthy. If the brain is impaired, these signals to the gut that promote these activities will be blunted.
The communication between the brain and the gut is heavily reliant on the vagus nerve! The vagus sends messages to the gut while also relaying messages about the gut environment to the brain. The vagus nerve communicates with the GI tract through the enteric nervous system, which is the gut’s exclusive nervous system.
I want to give you an overview of how the brain-gut axis can break down and cause SIBO. First, inflammation in the gut can cause damage to the nerves that produce the MMC. This inflammation will not only disturb the movement of food through the intestines (creating a very SIBO prone environment), but it will also generate inflammation in the brain. The brains ability to activate the vagus nerve will then become blunted by the inflammation in the brain, which will reduce blood flow, nutrients, enzyme release and motility in the gut leading to more inflammation in the gut! The process becomes a very vicious cycle of inflammation and dysfunction.
I want to go more into depth on this vicious cycle of inflammation. A good example of how gut inflammation can trigger brain inflammation is the food poisoning model for SIBO. Dr. Pimentel has elucidated that some cases of IBS and SIBO originate from a past food poisoning event. When you have food poisoning, your immune system develops antibodies to fight the toxins produced by the micro-organisms that have invaded the body. The toxin that is associated with IBS and SIBO is cytolethal distending toxin or CdtB toxin.
While the antibody helps remove the toxin from the body, it also has a striking resemblance (aka molecular mimicry) to a protein called vinculin that are found in the interstitial cells of Cajal and myoenteric ganglia (bundles of nerve cells). These cells innervate the gut allowing the smooth muscle of the gut to contract.
Shit really hits the fan (pun intended) when your body starts mistaking vinculin as the CdtB toxin. This auto-immune attack of your own vinculin will damage the nerves in the smooth muscle of the GI tract and reduce the ability of the cells to carry out their digestive functions. When these cells that are necessary for producing the MMC between meals atrophy, SIBO is eminent.
Food poisoning is only one way that nerves along the GI tract can be damaged. Datis (yes we are on a first name basis…or at least I wish we were) states that IBS, celiac disease, leaky gut, stress and IBD can all cause direct damage to the nerves that innervate the GI tract. All of this inflammation and lack of blood flow to the gut will compromise the gut barrier. As foods and bacteria start sneaking into the body, the immune system becomes overwhelmed and starts seeing everything as the enemy. The friendly fire of the overzealous immune system leads to tons of food sensitivity issues.
Once this inflammatory process starts in the gut, the immune system in the gut release cytokines that are messenger molecules that promote a systemic inflammatory response. The brain receives the cytokine message from the gut and activates the microglial cells of the brain. In addition, Lipopolysaccharide molecules, endotoxins produced from gut bacteria, will also have access to the blood stream and activate microglia in the brain.
Microglial cells are the brains immune soldiers that protect it from infectious agents. Once activated these cells are pro-inflammatory and will increase the immune response by releasing more inflammatory cytokines!
These microglia generate brain inflammation that cause neurons in the brain to fire more slowly. This neuroinflammation leads to symptoms that are quite prevalent in the SIBO community like brain fog, slower mental speed, slower recall and slower reflexes. The scariest aspect about activating these microglial cells is that they don’t have a built in off switch. Over time, these over-activated microglial cells will result in brain tissue damage and brain degeneration.
All of this neuroinflammation from the brain will compound gut inflammation, because ability of the brain to activate the vagus nerve will be impaired. Low vagal activity will reduce the MMC action, which will decrease motility and valve control in the gut. In addition, the vagus is also responsible for the release of digestive enzymes and bile into the gut, so the chemical process of digestion will be weakened.
Therefore, this brain inflammation creates the perfect environment for SIBO to thrive. Poorly digested food hangs out for long periods of time in the small intestine ripe for fermentation by gut bugs.
To make matters worse, the malfunctioning of the ileocecal valve can cause major problems. The ileocecal valve is the gateway that separates the small and large intestines. If the IC valve is not closing properly from local nerve damage and poor vagal activity, colonic bacteria will move up stream into the small intestine. Gut distention from fermentation will hold the valve open even further!
To sum up, inflammation from gut problems creates this vicious cascade of inflammation and dysfunction in both the brain and the gut. It will be impossible to heal from SIBO if you don’t have a healthy brain and strong innervation of the gut. The figure below may help you visualize the process.

My buddy, Datis, says we should all look at SIBO as a “complex web” that needs to be untangled. He is so right! To truly recover from SIBO, you need to address both gut and brain inflammation. I think SIBO is considered a relapse disease, because we usually fail to address the brain. The good news is there are some great strategies that you can take to repair the brain!
How do you know if your brain-gut axis is compromised?
First, it is important to determine if you have a compromised gut-brain connection. Here are a number of different options to give you some clues about the health of this gut brain axis:
1.Say Ahhhhh. You know at the doctor office when they ask you to “say ahhhh” and then look at the back of your throat. Well it turns out they aren’t just being annoying, they are actually looking at how your vagus nerve is firing! For this test, it may be easier to have someone look into the back of your throat rather than you trying to do it yourself. Oh and you need to dig up a flash light so they can see what’s going on back there.
So, what are you looking for? In the back of the throat, you can see the uvula (aka the lil dangly thing) and the soft palate. When you say ahhh, the soft palate should elevate and your uvula should remain at midline. A problem with the vagus nerve will manifest if the uvula deviates to one side and/or the soft palate doesn’t elevate on both sides equally. Here is a youtube video of a doctor testing the vagus nerve. I also have one of my famous drawings below to illustrate what should be happening.
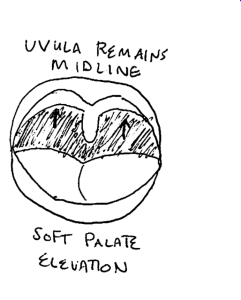
2. Gag reflex. The vagus also controls the gag reflux. A problem with the vagus can manifest as both a hyperactive gag reflex or a hypoactive gag reflux. You can test this with a tongue depressor or have your doctor test your reflex.
3. Bowel sounds. Datis has also recommended that bowel sounds can be diagnostic of low nerve activation through the gut. In a healthy person, you should hear a continual and cyclical growling tone when you listen to the bowels with a stethoscope. In someone with poor innervation of their GI tract, bowel tones will be greatly reduced and you will hear very infrequent rumblings. You can ask your doctor to do this or here is a great video to help you if you wanted to do this at home with a stethoscope.
4. Swallowing difficulty. The vagus controls the innervation for the swallowing process. If you struggle to swallow pills and supplements, this could be a clue that your vagus signaling is poor.
5. Antro-duodenal Manometry. This test can measure the MMC output in the small intestines. This test is the most direct way to test the function of the MMC in the gut, but unfortunately it is not widely available. There is no harm in asking your doctor to run this test though.
11 Tips to Repair Your Brain Gut Axis
1.Exercise your Vagus! Just like your muscles, neurons need constant stimulation to stay healthy and strong. If you break a bone and wear a cast for 6 weeks, it is almost shocking to see the muscle loss when they remove the cast. Because we didn’t use that muscle in 6 weeks it starts to waste away and lose its function. In the same way, neurons will start to lose their function if we aren’t actively working them out.
When we stimulate weak neurons, they start to build more proteins and become stronger. We can restore function in the brain gut axis by performing exercises that build positive plasticity and stronger connectivity in the vagal pathway.
Gargling is one of the best ways to build strength in vagal signaling pathway. The vagus nerve activates the palate muscles in the back of the throat that allows us to gargle. For this strategy to work, it is important to gargle vigorously! No half ass gargles allowed! Datis recommends that his patients gargle hard enough that they produce tears. You also want to gargle 2-3 times a day for a couple of minutes each time.
Singing can also activate the vagus, which is an awesome excuse to belt out some tunes in the shower or in your car. Singing isn’t quite as powerful as gargling for the vagus, so don’t skip the gargling.
Gargling and singing are like sprint exercises for your vagus, but your brain needs some strength training too. Gagging exercises with a tongue blade are equivalent to push-ups for the vagus. By combining all three of these exercises, it is like you are cross-training your vagus! You basically take a tongue blade and place it on the back of your tongue to induce the gag reflex.
When you first start doing these exercises, you may really struggle to gargle or to gag. This difficulty can be very diagnostic that your brain-gut axis is disturbed. As you work out the vagus and strengthen the neurons, gargling will become much easier. But, it does take weeks to build strength in this pathway. Just like it takes time to build six pack abs and huge biceps, building strong neuronal connections takes time. So, don’t get discouraged if you feel like an idiot choking on water in your kitchen….it happens to the best of us!
This video of Datis explaining these exercises might be helpful!
2. Coffee Enemas. Distending the intestines with a coffee enema can strengthen the nervous signaling in the gut. A bonus benefit is that enemas stimulate the contraction of the gallbladder, which helps detoxification of the liver.
The key to using coffee enemas is to hold them in the colon for as long as possible (Datis says to aim for 5-10 minutes) and to resist the urge to poo. When held in the colon, the caffeine in the coffee acts on the cholinergic receptors of the gut and stimulates the vagal pathway. Overtime as the vagal pathway becomes restored, Datis’ patients notice an increase in bowel function.
I have to admit that coffee enemas definitely intimidate me. I have never done one personally, but I have friends who swear by them! But, if you are having sluggish bowels, this may be worth a try.
3. Turn off the microglia! Once these immune soldiers of the brain turn on, they can’t be turned off. Even more problematic, they start recruiting other microglia for their pro-inflammatory crusade. There are a number of different plant compounds that can help attenuate microglia activation. These include: apigenin, luteolin, baicalein, resveratrol, rutin, catechins and curcumin. Personally, I have had success with brain symptoms by taking resveratrol and curcumin (not together but at different points of time). Both of these compounds are widely available. I really like this brand of curcumin.
4. Eat a whole foods anti-inflammatory diet. When you are having a problem with your gut brain axis it becomes imperative to remove processed foods from your diet and to increase your consumption of nutrient dense whole foods. Fruits and vegetables are filled with phytonutrients that can help calm systemic inflammation. Fatty fish high in omega 3 fatty acids like DHA are critical for brain health and have even been shown to increase vagus nerve activity.
Avoiding gluten is also important since it can promote intestinal permeability and inflammation in the GI tract. In addition, removing food sensitivities or trigger foods during the gut repair phase can also help calm the storm.
5. Make stress management a priority. Chronic stress breaks down the blood brain barrier. With this barrier compromised, the brains immune system will generate inflammation as it reacts to compounds and toxins that shouldn’t be allowed into the brain. Chronic stress also creates chronic activation of the sympathetic nervous system that is responsible for our fight or flight responses. This sympathetic activation will reduce blood flow, immune function and motility through the gut. Therefore, chronic stress can lead to inflammation and permeability in the gut.
Interestingly enough, the vagus nerve activates the parasympathetic nervous system that tells our bodies to rest and digest. Strong vagus nerve function can makes us more resistant to stress. Incorporating meditation, nature walks, yoga and other mindfulness activities into your daily life can help you build your stress tolerance.
Personally, I have just started meditating this summer and I have already noticed a boost in my cognition and stress tolerance. The stress of SIBO can be a lot to deal with so trying to find ways to laugh and destress with loved ones also helps a lot!
6. Get moving! Exercise increases the synthesis of a protein called BDNF (Brain Derived Neurtropic Factor). This protein is responsible for maintaining healthy neurons and creating new neurons. This increase in BDNF is suggested as the reason why exercise has been shown to drastically reduce inflammatory brain conditions like depression and anxiety.
Datis recommends choosing exercise that activates the coordination and balance centers of the brain while increasing blood flow to the brain. Treadmills and sedentary bikes don’t make the cut. But, yoga appears to be one of the best options for exercise, because you not only work on balance and coordination, but it can also help with stress management.
I was watching this comedy special recently and the comedian (I forget his name) made this joke: “yoga is just trying not to fart while stretching.” There has never been truer words spoken. That joke would have killed with a SIBO filled audience…but I digress.
7. Manage your blood sugar. Chronic surges of insulin and high blood sugar cause brain inflammation. When you have high blood sugar, the sugars in the blood start to stick to proteins and impair their function. This process is called glycation. Overtime, the end products from glycation start to destroy the nerves in the gut.
If you find that you feel tired after meals or that you are constantly craving carbohydrates, it could be a sign that you are having blood sugar issues. Asking your doctor to test your fasting blood sugar and your hemoglobin A1C may be a good idea if you have these symptoms.
8. Address thyroid issues. The vagus motor nuclei in the brain stem that activates the vagus nerve is saturated with thyroid receptors. Without enough active thyroid hormone (T3), vagus nerve stimulation to the gut will be suppressed. This compromises motility through the gut. That’s why it is so common for people with hypothyroidism to be chronically constipated. Working with a practitioner to address any thyroid dysfunction will help with brain-gut axis issues.
9. Don’t fear FODMAPs! As I have written before, I am not a huge fan of the FODMAP diet. I don’t think the FODMAP diet is good for the long term health of your colonic bacteria, but I hadn’t thought of the potential damage a low FODMAP diet could do to your brain until Datis blew my mind yet again!
When our gut bugs ferment fiber, they produce short chain fatty acids that serve as fuel for the brain. A short chain fatty acid deficiency has the potential to promote neurodegeneration in the brain. This increased neurodegeneration can result in decreased vagal output and impaired MMC activity to the gut. Again, it perpetuates this vicious inflammatory cycle along the brain-gut axis.
Obviously, there is a fine line when it comes to diet. You don’t want to eat trigger foods and a short term avoidance of FODMAPs may be helpful in reducing gut inflammation. But, being too restrictive and failing to add prebiotics back into the diet when the SIBO is cleared could promote this vicious cycle of brain-gut axis inflammation.
10. Probiotics. As I discussed in my probiotic article, a healthy large intestine is needed for a healthy small intestine. The bacteria in the large intestine communicate with the vagus nerve and can prompt its activation. You need a healthy population of colonic bacteria to stimulate MMC activity. Probiotics are transient micro-organisms that change the environment in the GI tract to facilitate the growth of good bacteria while inhibiting the growth of pathogenic bacteria.
You can get probiotics from fermented foods or supplements. If you have a histamine issue, you may want to avoid fermented foods and go with a supplement.
11. Vagal Nerve Stimulation. There are devices that stimulate the vagus nerve that are available for purchase. They are pretty expensive, but you can check out this Chris Kresser article if you want to learn more!
What About Prokinetics?
Both natural and pharmaceutical prokinetics are commonly used during SIBO treatment. Prokinetics stimulate the MMC and can therefore be a good tool to use at the start of treatment to help you get over the initial SIBO hump. While these MMC stimulators can help keep the gut functioning and the intestines clear of SIBO, they are not going to restore the underlying damage in the brain-gut axis. They are band aid fixes to the gut-brain axis problem.
I want to be clear that I do think prokinetics can be very helpful in the initial phases of the SIBO havoc! But, sometimes I think we can rely too heavily on prokinetics and fail to address brain-gut axis repair. I think the goal should always be to reboot our brain-gut axis’ own ability to generate MMC activity. The amount of prokinetic support needed is going to vary on a case by case basis, but I believe working on the brain-gut axis while on the prokinetic could make it much easier to wean off of it and lead to better long-term outcomes.
Final thoughts:
Don’t neglect the brain in your SIBO treatment!
I would love to hear about unique ways you are working out your brain-gut axis! Please leave a comment and let me know what’s up.
Stay tuned for future posts!
And please like the SIBO DIARIES FACEBOOK page so that you don’t miss any new posts! Click here to check out the Facebook page.
Want to address your brain gut axis dysfunction and other root causes with a SIBO knowledgeable practitioner?
I can help!





Many many thanks for such an enlightening arricle
Kind regards
Sonia
Awww! Thanks for reading Sonia!
Thanks for putting all of this together in such an easy to understand and thorough way. I saw Datis for neuro and SIBO and the coffee enemas and vagus nerve focus were game changers for me. I don’t think my body would have lasted much longer on the killing bacteria focus that my GI doc had me doing. I was wasting away. After one month of following the vagus nerve protocol, I had significant change. I really appreciate the brain inflammation piece because that is a huge part of what throws my progress off and I have to keep revisiting the things to calm it down.
Wow!! Thanks for sharing your experience Tiffany! I definitely think focusing on brain could be a game changer for so many other people! I am so jealous you got to work with Datis in person! I’m sure he was amazing to work with!
Hello,
I’m the mom of a child with SIBO who also has sensory processing disorder. I, too, believe these to be symptoms of something else.. She’s been seeing an occupational therapist who has diagnosed her with “retained primitive reflexes” which are linked to all kinds of postural, motor, digestive, and sensory difficulties. My daughter does daily exercises to address the retained primitively reflexes, and I’m hopeful this will address some of these other isssues as well. What do you think?
Now it all makes sense and I can exactly relate my symptoms to the findings. One thing I have also noticed and is complimentary to the findings is posture. When I am slouched on the couch my depression worsens. As opposed to sitting upright with support which alleviates depression symptoms. I suppose having a straight vagus nerve frees up the communication pathways. This is my hypothesis but I bet you I am right. Something to consider for your treatment. Wishing everyone success on their journeys and a big thankyou to all those that have helped us folks heal.
In 11/16 I purchased a device called Bemer for my fibromyalgia and it helped me significantly (all this while at the stage of self-treating SIBO while awaiting Dr evaluation). It helped fibro dramatically (premise of this is a separate story). For the past 3 days, I have specifically used a certain Bemer applicator directly down the spinal chord for 8 minutes, twice daily and notice a difference already to vagus function.
Also, one interesting note about this article is the premise of molecular mimicry, which reminds me of molecular imprint, something I would describe as the premise of homeopathy (I am a homeopath btw).
I have a Bemer, but have not used it on a regular basis. Could you let me know what settings work best for you and if you use the large mat or small applicator.
I have struggled with SIBO for 10 years (misdiagnosed for the first 8). I have done every diet known to the SIBO world, and they all made me worse… I just get sicker by the day. I may have read 1000 articles on SIBO and this might be the BEST EVER. I am almost in tears. My therapist, who I see more often when SIBO flares up due to increased depression and anxiety, suggested I read a book on brain health She is the second Mental Health Practioner who said “you are not crazy, this is connected to your SIBO”. I live in a small town and oddly have amazing Mental Health support, but not a single Functional Medicine doctor (or anything close). Traditional treatment made me worse, diets made me worse, and all along I knew intuitively what you’ve said here, but didn’t have the connections I needed to fully understand what I felt. This article has helped me more than words can express. Thank you!
Thank you so much for your kind words! I am so happy my blog has helped you sort through all the SIBO craziness! Best of luck in your health journey!
Heather, just wanted to reply because we have a lot in common! I’ve had SIBO for 7 years after sustaining a brain injury, but only last year was I finally able to be diagnosed. I have tried everything with food and diets on my own- year after year of trying and failing and feeling despair. . I have watched all the SIBO Summit videos and am overwhelmed with trying to decide whether to start with a new doctor remotely, or sticking with the only naturopath in my whole state who knows what SIBO is but doesn’t really know how to help me with the food aspect of it, or the vagus nerve aspect of it. Like you, I have a lot of anxiety and depression that go along with it, but I had attributed them to the brain injury and not the SIBO. All I know is that I have not felt the same mentally since it happened. Just wanted to say hi since it gets pretty isolating feeling like this.
Excellent information on SIBO
Thanks so much for reading!
This post is FANTASTIC! I came across your link on one of the SIBO support groups and I’m so glad I did! Thank you for sharing such knowledgeable information. 🙂
Thanks Hannah!! I’m so happy you found this post helpful!
I did the say ahhhh test and it was normal. I’m SIBO C and do yoga everyday. Would you suggest still incorporating the gargling, singing and gagging exercises? Do you have a trusted source of coffee enema instructions that you could share? Thank you so much for all of the information and experience that you share on your blog. You are doing a great service to many suffering people and you are appreciated for your service.
Peace, Tiffany
Hi Tiffany!! Thanks so much for reading and the kind words.
On whether to do the exercises or not, it really depends on whether you suspect a breakdown in your vagal function. I would say trying the exercises for 2-3 weeks and seeing how you feel would be a good experiment to see if you really have any brain-gut axis dysfunction. If you notice a benefit in gut function, than those exercises can be continued, but if you don’t than you might need to address some other underlying cause to correct your SIBO.
As far as coffee enema resources, here is a good article: https://metabolichealing.com/coffee-enemas-benefits-guidelines/
Best of luck tiffany 🙂
I have SPMS any advice for me? I was diagnosed in 2012
How to repair the brain-gut axis? It all starts with the Vagus! | THE SIBO DIARIES
[…]You want to realize that nobody medicine goes to work for everybody who has PTSD.[…]
This is an excellent article, I’m wondering if this vague nerve is what causes colitis?
A great post, especially for one with a hyper-inflammatory gut and multiple allergies. I shall discuss it with my naturopath and serif we can start moving forward. Thank you for the clear explanations.
I am so glad you found this post helpful! I hope you and your naturopath can find good strategies to address your brain-gut axis 🙂
Your information is a God send to me. I have had IB S for 44 years (probably Sibo) and have been to countless types of doctors including to Mayo Clinic. My health has progress lively gotten worse to the point where I was in a very deep out of pain and depression.
I do find of research and have made some recovery but am not cured of this nasty SiBO yet. Your article makes so much sense. I have not read any of this in any depth where I could tackle it. I am now armed with new knowledge and ready to fight on. Thank you from the bottom of my heart.
Marilyn
Wow! Thanks so much for the kind words Marilyn! So happy that my article was helpful 🙂
Excellent write up. I had already suspected vagus nerve function a year before I was formally diagnosed with SIBO this July, and started working on strengthening it mainly through exercising the gag reflex, diaghrammatic breathing and cold showers. I have always had low BP, syncope in my teenage and faint easily when dehydrated, and developed IBS around the same time when I started smoking 30 years back.
I stopped smoking two years ago, which triggered gut issues at night (bloating/burping all night), developed gluten sensitivity and lost 20lbs. I was put on an antidepressant for sleep instead of fixing the gut issues. In Feb this year, I stopped the meds, which led to rebound insomnia and GI flare up and I suffered for 6 months, and lost 40lbs, before I was put on anti-microbials for SIBO. I just finished my treatment and my gut is mostly calm although I have to avoid gluten, dairy and sugar due to food sensitivity. I also started yoga in July and that has been truly transformative in my healing journey.
I am still dealing with fragmented sleep although I able to get a contiguous block of 4-5 hours before my gut wakes me up. One interesting symptom when I wake up, is the firing of thoughts accompanied by gut activity. I can hear, feel and experience all the sensations but when I open my eyes, an hour has passed. It’s almost like rem sleep fully awake. I also have some daytime anxiety and fears that switches off like magic in the evening. I don’t know if it’s a remnant of antidepressant withdrawal impacting the brain or still gut related.
Incidentally I did the “aah” check today and I noticed that my uvula on the right side doesn’t go up like the left side, and there appears to be a dark line on top that almost feels like a vein or blood clot. Do you have more information on how that relates to vagus nerve function? And of that is something that gets fixed by exercising the vagus nerve or is a condition that must be managed?